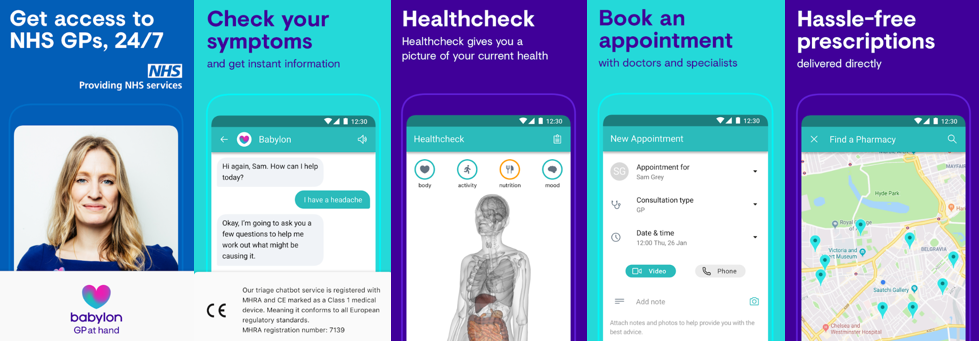
Just imagine a very familiar scene: 3 a.m. and you google your symptoms and self-diagnose your illness. Then you have to decide based on whatever search has come up whether or not you need to see a doctor. This is one of those times where AI chatbots come into play. More and more HealthTech companies are focusing on providing a software solution for patients to define symptoms and then get proper treatment. Triage chatbots is an alternative to googling your symptoms. A user can enter the main complaints and will then be asked a number of questions based on the given info. At the end of a session, the bot suggests the way to treatment. Chatbots can initiate video chats with real doctors, direct to patient booking systems or just advice where to ask for help. For the most part AI chatbots are intended to support physician workflow rather than replace them anytime soon. The key concept is to relieve the burden on physicians and medical teams. In fact, chatbots have limited authority. Indeed, the U.S. Food and Drug Administration does not allow an app to diagnose a patient or prescribe drugs without physician input. However, Joel Barthelemy, founder and CEO of Arizona-based GlobalMed, is sure that is to change in the near feature. Today?s AI-enabled apps, based on the experience of many thousands of similar patients with the same symptoms, can suggest doctors which medication to prescribe or which treatment to try. As software shows more accurate results, physicians will agree with these apps most of the time unless they know something unique about their patients. Then they can contact a patient and ask more specialized questions. But Mr. Barthelemy claims that, in most cases, patients will no longer have to see primary care doctors in person.
AI and chatbots in healthcare: case studies
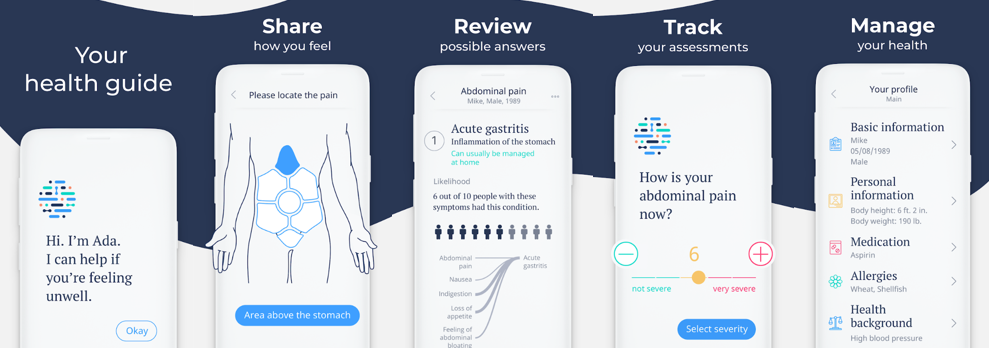
Ada Health
?s mobile software is described as ?a personal health companion and telemedicine app?. Users can figure out what symptoms they have via Ada?s conversational interface and get info on what might be the cause. If necessary, Ada then offers a follow up remote textual consultation with a real doctor.
?Ada has been trained over several years using real world cases, and the platform is powered by a sophisticated artificial intelligence (AI) engine combined with an extensive medical knowledge base covering many thousands of conditions, symptoms and findings,? the company explains.
?We designed the PD Coach to address specific challenges that Parkinson?s patients and their caregivers may face ? including its unique ability to learn and adjust to language and vocabulary for patients with dexterity and speech issues,? Mike Davis, head of UCB?s US Neurology Patient Value Unit, said. ?With insights from patients on the challenges they face with disease management, April was created as more than a resource to offer information. April is designed to build a relationship with the patient and help deliver what patients value when it comes to their care.?
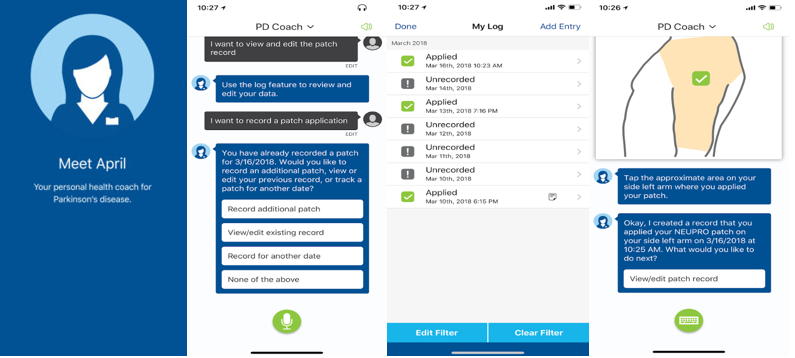
“This AI and automation-powered technology creates a new avenue for patients to turn to for help and guidance that has the convenience of an app,? Michael Southworth, general manager of intelligent self-service at Verint, said. ?AI and intelligent assistant technology has the ability to transform healthcare and access for patients. With April, we?ve built a resource that can truly meet patients where they are and allow them to take greater control of their health.?
AI in healthcare apps: criticism
AI-enabled chatbots are not without controversy. A study from MIT computer scientists suggested that AI can?t provide the same quality of care as physicians. The researchers analyzed doctors? written notes on intensive care unit patients and found that ?internal sensations? about a particular patient?s condition played a prominent role in determining how many tests should the patient have.
?There?s something about a doctor?s experience, and their years of training and practice, that allows them to know in a more comprehensive sense, beyond just the list of symptoms, whether you?re doing well or you?re not,? Mohammad Ghassemi, a research affiliate at IMES, said. ?They?re tapping into something that the machine may not be seeing.?
Conclusion
Artificial intelligence now has a deeper touch in healthcare. AI-powered chatbots can diagnose patient conditions via mobile devices. The technology allows caretakers and doctors to remotely monitor the elderly and critically ill patients. The potential of AI in healthcare is both promising and alarming, considering the possible effects of one bad decision. Therefore, AI-powered software should earn its credibility in the eyes of physicians and patients. For instance, AI chatbots might support human decision making while providing a recommended treatment plan. Maybe in the distant future, a chatbot will replace a flesh-and-blood doctor. But today?s AI-powered solutions are not sufficiently effective lacking a doctor?s gut feeling. Supporting Resources: https://www.healthcareitnews.com/news/next-gen-telehealth-ai-chatbots-genomics-and-sensors-advance-population-health https://techcrunch.com/2017/04/19/ada-health/ https://www.businesswire.com/news/home/20181115005077/en/UCB-Verint-Announce-Launch-UCB%E2%80%99s-PD-Coach http://news.mit.edu/2018/doctors-rely-gut-feelings-decision-making-0720